The amyotrophic lateral sclerosis (ALS) diagnostic journey is unique to each individual. It has puzzled neurologists, been mistaken for allergies or back issues by physicians, stressed out families, and most significantly, it has prevented patients from knowing what is affecting their body.
The median diagnostic delay for a person living with ALS is 12 months (Martharan, 2020). In other words, from the time of their first symptom onset, it takes roughly a year to positively diagnose someone with ALS. Not only that, but each person living with ALS sees an average of three different physicians before receiving their ALS diagnosis (Paganoni, 2014). In the world of rare diseases, this diagnostic delay is not uncommon, but on a patient level, this lag can be life threatening. Not only does the delay prevent patients from seeking the correct medical attention for their symptoms, but it also reduces the time frame a patient has to enroll in clinical trials.
So, if it really takes a year to get diagnosed with ALS, where does all the time go? According to peer reviewed literature, there are three key stages that have quantifiable lags (Paganoni, 2014).
-
- Time from symptom onset to the first doctor visit: 4 months
- Time from the first doctor visit to a suspected ALS diagnosis: 3 months
- Time from suspected to confirmed ALS diagnosis: 1 month
Research studies have also been conducted to analyze what factors delay or accelerate an ALS diagnosis:
-
- Patients age 60 and older: delayed ALS diagnosis
- The presence of fasciculations, slurred speech, and lower extremity weakness when symptoms are first noted: accelerated ALS diagnosis
- Sporadic ALS and limb onset: delayed ALS diagnosis
If we analyze the above diagnostic delay predictors in each individual ALS case, we can start to break down what really is at the root of a delayed diagnosis. Was it the patient’s stubbornness and refusal to go to the doctor? Was it a primary care physician failing to identify the patterns of a highly complex disease or not wanting to give a fatal diagnosis? More than likely, it was a culmination of multiple variables. The author of this blog has identified four key categories of dysfunction that influence the ALS diagnostic process: public knowledge, the medical system, the pharmaceutical industry, and ALS disease complexity. There are specific failures within each category. The charts below list these points of failure.

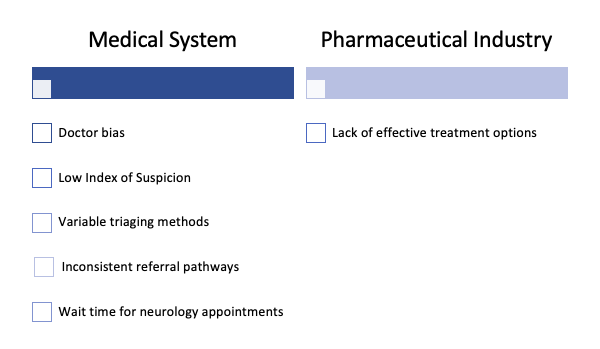
Compensating for each of these system failures will take, and is taking, years and millions of dollars. Is there a simpler solution? Or do we approach each of these system inefficiencies individually? Yes, there is a simpler solution. Machine learning is proving to be the solution. Mitsubishi Tanabe (MT) Pharma, the company known for developing the ALS therapy, endaravone, is hard at work. They have created a program that interfaces with billing codes within our medical systems. The software is trained to identify potential ALS patients before they receive their ALS diagnosis. How is this possible? MT Pharma acquired historical claims data on Truven from 14,000 ALS patients during the 5 years leading up to their ALS diagnosis. They looked for patterns in the billing codes and created an algorithm to detect similar patterns. This early detection software was in the beta testing stages in December 2019 and will hopefully be utilized in the near future. The early stage testing results revealed the software had a 14% positive predictive value. In other words, roughly 1 out of every 9 people who were flagged by the system were correctly identified as having ALS. This early detection method not only has implications in ALS, but in the larger populations of patients at risk of developing neurodegenerative diseases such as Parkinson’s and Alzheimer’s.
This solution to the ALS diagnostic delay highlights two important points: it warns the public that they should never underestimate a pharmaceutical company’s ability to find customers, and it reveals that rare disease populations can benefit from pharmaceutical marketing budgets. Does this solution imply we should stop working on the systematic inefficiencies that allow patients with rare diseases to fall through the cracks? Absolutely not. Leslie Sands is living with ALS in San Luis Obispo. These are her recommendations for medical professionals everywhere:
-
- A local specialist or primary care physician (PA’s and NP’s included) should urgently refer their patient to a university or a major hospital neurology center for evaluation when: they encounter a patient with unexplained slurred speech and have ruled out a stroke, traumatic brain injury, or other “obvious” conditions, and the patient’s labs are inconclusive with no obvious alerts.
- The local doctor should not “suggest” that the patient seeing a neurologist associated with a university or major hospital may be a good idea; rather, the local doctor should emphasize the importance of seeing a qualified neurologist.
- The local doctor or specialist should not be afraid to broach the possibility of a motor neuron disease (MND).
Leslie’s recommendations are echoed by ALS researchers who have collected data on patients who received a diagnosis far too delayed into their disease experience. One incredible ALS advocate, Sandy Morris, recommends that anyone who thinks they may have ALS symptoms, goes to a local emergency room and doesn’t leave until they receive a diagnosis. Hey, that’s one way to do it.
As with most complex problems, it is a combination of disciplines that need to collaboratively work towards a solution. While ALS patients encourage medical professionals to heighten their awareness of ALS, MT Pharma’s early detection algorithm will assist the doctors with the pattern recognition needed to correctly diagnose neurodegenerative diseases.
Related Articles:
Diagnostic Delays in ALS ‘Surprisingly Large’ and Need Not Be, Study Says
References
Martharan, Martin, Mathis, Stephane, Bonabaud, Sarah. (2020). Minimizing the Diagnostic Delay in Amyotrophic Lateral Sclerosis: The Role of Nonneurologist Practitioners. Neurology Research International. Volume 2020 Article ID 1473981, 8 pages.
Paganoni, S., Macklin, E. A., Lee, A., Murphy, A., Chang, J., Zipf, A., Cudkowicz, M., & Atassi, N. (2014). Diagnostic timelines and delays in diagnosing amyotrophic lateral sclerosis (ALS). Amyotrophic lateral sclerosis & frontotemporal degeneration, 15(5-6), 453–456.

